June 24, 2010
Largest ever interprofessional training event for health sciences students a success
According to a 2007 study by the Agency for Healthcare Research and Quality, teamwork breakdowns, such as lack of supervision and patient hand-off problems, account for 70 percent of errors by medical trainees.
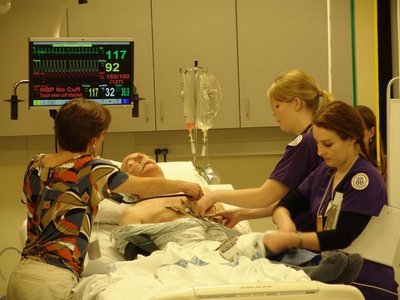
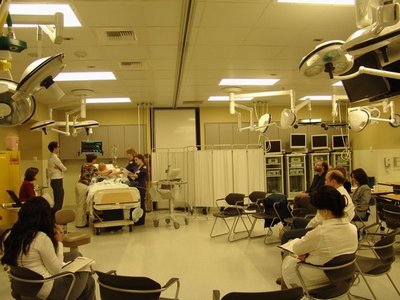
For the first time ever the UW’s schools of medicine, nursing, and pharmacy have partnered in a clinical simulation lab to practice their patient safety and team communication skills.
“Working with other medical disciplines made the simulation more realistic and at several points during the simulation it felt real,” said Ken Sheil, a physician assistant student. “The simulation allowed us to interact as if we were all licensed and working. I feel more of this type of training prior to our clinical year and during our clinical year would be beneficial.”
This was the first time students from these disciplines have collaborated in a simulated clinical setting. Students in most health care disciplines train separately, despite the fact that the very colleagues they’ll later work with are learning about the same conditions just a building wing or two away.
After each simulated exercise, the interdisciplinary teams debriefed on the clinical issues encountered during the training, and discussed the effectiveness of the team’s communication. By far, the overall student experience was most significantly enhanced by the opportunity to work alongside other disciplines in a mock clinical setting. “We should so this every week,” said Jeanette Kelly, a medical student who led a team through a scenerio simulating a patient with an excessively high heart rate.
Getting medical, nursing, physician assistant, and pharmacy students excited about the idea of working together as a team helps break down hierarchal barriers. Training together builds mutual respect. It also helps establish good communication patterns and a team approach to health care that will stay with them throughout their professional careers.
A group of 20 students from various UW health sciences schools met with faculty members to develop clinical scenarios for the simulations last year. The interdisciplinary training was part of the School of Medicine’s weeklong capstone program created to refresh medical students skills as they transition to residency training. The capstone program includes various elective sessions on intubation, IV placement, basic airway management, and many other common clinical procedures.
The interprofessional skills project team included principal investigator Brenda Zierler from the School of Nursing, co-principal investigator Brian Ross from the School of Medicine; Doug Brock, Tom Gallagher, Grace Landel, Karen McDonough, all from the School of Medicine; Sara Kim, School of Dentistry and School of Medicine; Nanci Murphy and Peggy Odegard, School of Pharmacy; and Sarah Shannon and Diana Taibi, School of Nursing.
Julie H. Case, managing editor of the UW Alumni Association’s Columns magazine, contributed to this story.